If you haven’t heard of eugenics (meaning “well-born”), it is the study of or belief in societal and scientific intervention to bring about the “fittest” population through means such as forced sterilization, abortions, euthanasia and discriminatory marriage laws. The movement’s intent was to improve the quality of the human population by discouraging reproduction by people with genetic defects or what were thought to be inheritable undesired traits.
The origin of eugenics in the United States began in 1899 with Albert Ochsner, future Professor of Surgery at the University of Illinois. In his published paper Surgical Treatment of Habitual Criminals, Ochsner described a new procedure that sterilized a male subject by cutting his vas deferens, a procedure that became known as a vasectomy. He advocated for the use of vasectomies on criminals, believing that:
 The height of the eugenics movement (1920s to mid-20th century) saw compulsory sterilization programs established in over 30 states, resulting in over 60,000 sterilizations of often healthy people. Criminals and prison inmates were especially targeted, as well as those deemed “feeble-minded,” mentally deficient, or simply capable of passing on undesirable genes.
The height of the eugenics movement (1920s to mid-20th century) saw compulsory sterilization programs established in over 30 states, resulting in over 60,000 sterilizations of often healthy people. Criminals and prison inmates were especially targeted, as well as those deemed “feeble-minded,” mentally deficient, or simply capable of passing on undesirable genes.
Planned Parenthood, a global reproductive health care provider, was actually a product of the eugenics movement. Its founder, Margaret Sanger, was a prominent eugenicist who argued that this “new weapon of civilization and freedom” could solve “race problems” and result in “racial regeneration.” This belief in ensuring “racial purity” typically involved laws that aimed to prevent interracial marriage, taking the concept of eugenics and population control another step further.
If any of this sounds familiar, history’s most infamous admirer of America’s eugenics policies was Adolf Hitler, who modeled the Third Reich after American eugenic institutions. As he expressed in Mein Kampf, Hitler was determined to prevent “defective people” from “propagating equally defective offspring,” a mission that he firmly believed required a systematic execution. In response, the American Eugenics Society issued a statement of praise in 1937 to the Nazi scientists who hoped to cleanse the gene pool.
 MINNEAPOLIS, Minnesota — Dr. Steven Shu, founder of
MINNEAPOLIS, Minnesota — Dr. Steven Shu, founder of 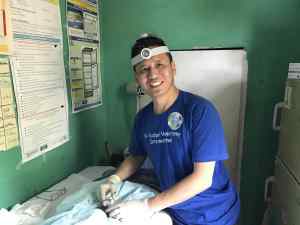 Dr. Shu, MD, MBA, is a cosmetic surgeon and proceduralist and founder of MVI and Surgeon Volunteers. Since joining No-Scalpel Vasectomy International, Inc (NSVI), an international medical volunteer organization led by urologists Dr. Doug Stein and Dr. Ramon Suarez, in 2014, Dr. Shu has completed six mission trips to Haiti and the Philippines.
Dr. Shu, MD, MBA, is a cosmetic surgeon and proceduralist and founder of MVI and Surgeon Volunteers. Since joining No-Scalpel Vasectomy International, Inc (NSVI), an international medical volunteer organization led by urologists Dr. Doug Stein and Dr. Ramon Suarez, in 2014, Dr. Shu has completed six mission trips to Haiti and the Philippines. Your doctor will test your semen approximately 12 weeks after your vasectomy to examine for presence of motile sperm. If test results show that your semen is sperm-free, then the vasectomy was successful, and additional birth control will no longer be necessary. Some patients’ semen may show a small number of non-motile sperm, whereby the risk of pregnancy is very low, and additional birth control may not be needed.
Your doctor will test your semen approximately 12 weeks after your vasectomy to examine for presence of motile sperm. If test results show that your semen is sperm-free, then the vasectomy was successful, and additional birth control will no longer be necessary. Some patients’ semen may show a small number of non-motile sperm, whereby the risk of pregnancy is very low, and additional birth control may not be needed.


